SLIDE 1
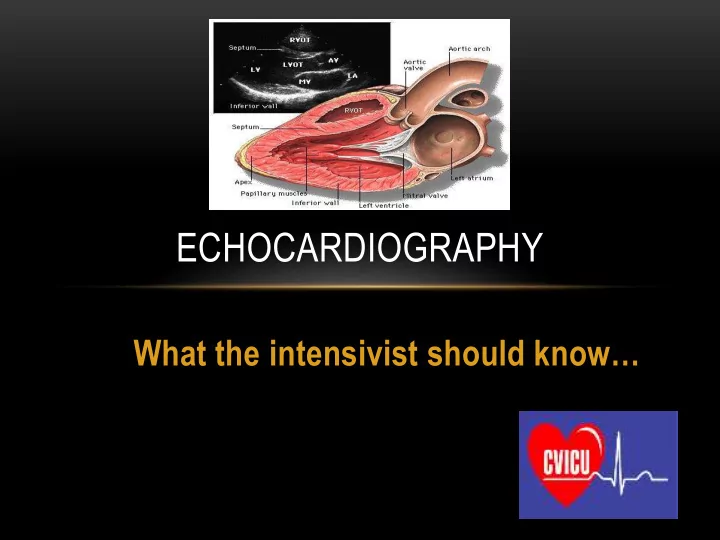
What the intensivist should know…
ECHOCARDIOGRAPHY

SLIDE 2 OVERVIEW
- Background
- Why ECHO?
- Limitations
- How to learn ECHO
- What you need to know
- Where we are heading

SLIDE 3
BACKGROUND

SLIDE 4

SLIDE 5
BACKGROUND

SLIDE 6
COLLEGE AKNOWLEDGEMENT

SLIDE 7 WHY DO WE NEED TO LEARN ECHO?
- Filling the void
- Differentiating shock
- Tamponade post cardiac surgery
- Management of cardiovascular supports
- ECHO in cardiac arrest

SLIDE 8 LIMITATIONS
- Scope of practice
- Impact of
- False positives
- False negatives
- Formal studies
- Advanced studies

SLIDE 9 HOW TO LEARN ECHO
- BOOKS
- COURSES
- WEBSITES
- HANDS ON SACNNING
- SUPERVISION
- POST GRAD CERT/DIPLOMA

SLIDE 10
WEBSITES

SLIDE 11

SLIDE 12 CICM GUIDELINE
- Attend an approved ECHO course
- Find a supervisor
- Perform 35 focussed cardiac ultrasound cases
- Record images/ Write in notes
- Complete and pass an online MCQ exam @CICM
- In the furture- there may be a ‘live’ exam

SLIDE 13 CICM GUIDELINE
- Basic physics
- Machine setup
- Patient details
- Image optimization
- Basic views (PLA/ PSA/ A4C/ Scand IVC)
- Focussed questions looking for pathology
- Limitations
- Colour/Doppler not included

SLIDE 14 CICM GUIDELINE- FOCUSSED QUESTIONS
- 1. Is the LV significantly impaired?
- 2. Is the LV dilated?
- 3. Is the RV function grossly abnormal?
- 4. Is the RV dilated?
- 5. Is there any pericardial fluid/tamponade?
- 6. Is the patient significantly hypovolaemic?
- 7. Conclusion addressing relevant clinical question

SLIDE 15

SLIDE 16

SLIDE 17 SHOCK ALGORITHM
- Assess volume status exclude hypovolaemia
- IVC
- LV EDV
- Assess contractility of LV exclude LV failure
- Exclude tamponade
- Assess right heart function exclude PE
- Exclude pneumothorax
- Exclude AAA
……..takes about 3 minutes….

SLIDE 18 CARDIAC WINDOWS
- Parasternal
- Long axis
- Short Axis
- Apical
- 4 chamber
- 2 chamber
- Subcostal


SLIDE 20
PARASTERNAL LONG AXIS

SLIDE 21
PARASTERNAL LONG AXIS

SLIDE 22
PARSTERNAL SHORT AXIS

SLIDE 23
PARASTERNAL SHORT AXIS

SLIDE 24
PSAX

SLIDE 25
PARASTERNAL SHORT AXIS

SLIDE 26
APICAL 4 CHAMBER

SLIDE 27
APICAL 4 CHAMBER

SLIDE 28
APICAL 4 CHAMBER

SLIDE 29
APICAL 2 CHAMBER

SLIDE 30
APICAL 2 CHAMBER

SLIDE 31
SUBCOSTAL

SLIDE 32
SUBCOSTAL VIEW

SLIDE 33
SUBCOSTAL

SLIDE 34 LV CONTRACTILITY
- Overview
- Visual ‘Gestalt’
- Fractional area change (FAC) (40-60%)
- Simpsons method
- Mild impairment EF 50-70%
- Moderate impairment EF 30-50%
- Severe impairment EF <30%

SLIDE 35
LV CONTRACTILITY- NORMAL

SLIDE 36
LV CONTRACTILITY- NORMAL

SLIDE 37
LV CONTRACTILITY- NORMAL

SLIDE 38
LV CONTRACTILITY- NORMAL

SLIDE 39
LV CONTRACTILITY- NORMAL

SLIDE 40

SLIDE 41

SLIDE 42
SIMPSONS

SLIDE 43
SIMPSONS

SLIDE 44

SLIDE 45

SLIDE 46

SLIDE 47

SLIDE 48

SLIDE 49

SLIDE 50

SLIDE 51

SLIDE 52

SLIDE 53

SLIDE 54

SLIDE 55

SLIDE 56

SLIDE 57

SLIDE 58

SLIDE 59

SLIDE 60

SLIDE 61

SLIDE 62

SLIDE 63

SLIDE 64

SLIDE 65

SLIDE 66

SLIDE 67

SLIDE 68

SLIDE 69

SLIDE 70

SLIDE 71

SLIDE 72

SLIDE 73

SLIDE 74

SLIDE 75

SLIDE 76

SLIDE 77 THE RIGHT VENTRICLE
- Shape
- Size
- Function
- Assesment

SLIDE 78
VOLUME AND PRESSURE OVERLOAD

SLIDE 79
RV/LV RATIO- NORMAL (0.6:1)

SLIDE 80

SLIDE 81 CLASSIC SIGNS OF PE
- Dilated RV
- Septal flattening
- Impaired RV
- Tricuspid regurgitation
- McConnels sign
- Raised PA pressures (RVSP)
- Visible clot

SLIDE 82

SLIDE 83

SLIDE 84

SLIDE 85

SLIDE 86

SLIDE 87

SLIDE 88

SLIDE 89

SLIDE 90
SEPTAL FLATTENING

SLIDE 91
SEPTAL FLATTENING

SLIDE 92
SEPTAL FLATTENING

SLIDE 93 VOLUME STATUS- IVC
- IVC
- Abdominal probe
- Sub-costal view- longitudinal
- Using liver as a window
- Measure IVC 2cm distal to diaphragm
- Collapsibility with respiration
- Visual gestalt
- M-mode

SLIDE 94
IVC DIAMETER AND CVP

SLIDE 95
IVC

SLIDE 96
IVC

SLIDE 97 IVC ANALYSIS
- Absolute diameter
- <1cm Correlates with a CVP ~ <5cm H20
- 1-2cm Correlates with a CVP ~ 5-15cm H20
- >2cm correlates with a CVP ~ >15cm H20
- Variability
- Ventilated patient
- >12% collapsibility indicates volume responsiveness
- Unventilated patient
- >50% collapsibility indicates volume responsiveness

SLIDE 98
VOLUME STATUS-IVC

SLIDE 99

SLIDE 100

SLIDE 101
VOLUME STATUS

SLIDE 102

SLIDE 103

SLIDE 104

SLIDE 105

SLIDE 106
LVEDA NORMAL 12-16 CM
2

SLIDE 107
LVEDA

SLIDE 108

SLIDE 109

SLIDE 110

SLIDE 111
‘KISSING’ PAPILLARY MUSCLES

SLIDE 112

SLIDE 113 PERICARDIAL EFFUSION AND TAMPONADE
- Is there a pericardial effusion/collection?
- <10mm
Small
Moderate
Large
- Is there evidence of tamponade?
- Hypotension
- RA or RV free wall collapse
- Dilated IVC

SLIDE 114

SLIDE 115

SLIDE 116

SLIDE 117

SLIDE 118

SLIDE 119

SLIDE 120

SLIDE 121

SLIDE 122

SLIDE 123

SLIDE 124

SLIDE 125

SLIDE 126

SLIDE 127

SLIDE 128

SLIDE 129

SLIDE 130

SLIDE 131

SLIDE 132

SLIDE 133

SLIDE 134
WHERE THINGS ARE HEADING

SLIDE 135 THE FUTURE
- Portable wireless probes
- Formal basic ECHO training and examinations in CICM
- Advanced ECHO clinician in every ICU
- In-house credentialling and CME
- TOE and disposable probes

SLIDE 136
What the intensivist should know…
ECHOCARDIOGRAPHY